Thyroid Eye Disease (TED)
A Complete Overview of Thyroid Eye Disease Causes, Symptoms, Diagnosis, and Treatments

Join Us for the 2026 TED Patient Forum >> Register
A Complete Overview of Thyroid Eye Disease Causes, Symptoms, Diagnosis, and Treatments

Thyroid eye disease requires attentive care from patients, family, and healthcare providers to achieve optimal outcomes.
Timely recognition and prompt care from your doctor can significantly impact the course of the disease and prevent serious complications. Full education full scope of this condition is important for everyone involved in care.
Thyroid eye disease (TED) is a progressive autoimmune inflammatory disorder that primarily affects the tissues surrounding the eyes.
Despite its name, thyroid eye disease is not solely a consequence of thyroid dysfunction but rather a semi-independent process driven by shared autoimmune mechanisms – an intricate relationship between thyroid function and ocular manifestations.
Appreciating the connection between autoimmune disease and thyroid eye disease helps explain why treating the thyroid alone may not resolve eye symptoms, and why these conditions need separate attention and treatment approaches.
Thyroid eye disease (TED) can cause serious complications including vision loss, persistent double vision, and permanent eye damage if not recognized and treated early. Intervention and proper management through both surgical and non-surgical approaches can greatly improve individual outcomes.
At Kahana Oculoplastic and Orbital Surgery, we pride ourselves on being on the cutting edge of surgical and therapeutic treatments for thyroid eye disease. We have unique knowledge, expertise, and passion for treating this disease.
We offer the latest non-surgical technologies, treatments, and a deep understanding of this particularly dreadful disease process.
The extent of surgical rehabilitation is customized and patient-specific. Coordination and proper sequencing of surgical intervention is key to promoting good outcomes
What is the difference and connection between these conditions.
Graves’ ophthalmopathy (also sometimes called Graves’ orbitopathy) is not the same as Graves’ disease.
These four fundamental characteristics of thyroid eye disease help doctors track progression and plan treatment. Understanding these characteristics helps predict how the disease might develop in individual patients.
The systemic impact of thyroid dysfunction can affect multiple body systems simultaneously. Understanding these widespread effects helps explain the variety of symptoms patients may experience.
Note: These symptoms, particularly mood changes, may be misdiagnosed as psychiatric disorders rather than recognized as effects of hyperthyroidism.
The connection between thyroid dysfunction and eye problems stems from shared immune system targets. This unique relationship explains why eye symptoms may persist even after thyroid function is controlled.
Thyroid eye disease most frequently occurs when the immune system attacks both the thyroid gland and the eye tissues, causing scarring, muscle enlargement, and fat expansion in the eye socket. The tissues of the eye share similar features with the thyroid and can respond to thyroid hormone levels. Though most patients with eye symptoms have abnormal hormone levels and antibodies, the condition can and does occur even with normal thyroid levels.
The thyroid and eye components of the disease each require separate treatments despite their common origin.
The anatomy of the eye socket plays a crucial role in how symptoms develop and progress. Because the eye socket is a confined space, even small amounts of inflammation can cause significant problems.
The confined space of the eye socket exacerbates the effects of inflammation and congestion. This anatomical context is critical to understanding why thyroid eye disease can lead to serious complications such as optic nerve compression and potential vision loss.
The team at Kahana Oculoplastic and Orbital Surgery are here to help. If you are experiencing symptoms, have questions, or are unsure of your condition, don't hesitate to contact us.



Recognition of both systemic and eye-specific symptoms is neccesary for proper diagnosis and personal treatment. The diverse range of symptoms reflects the complex nature of this autoimmune condition.
These symptoms may not always indicate thyroid eye disease, but they warrant prompt evaluation by an eye specialist.
Thyroid eye disease (TED) typically progresses through phases over time. The first phase, known as the active or inflammatory phase, lasts approximately 6-24 months and is characterized by active inflammation and tissue changes.
During this period, symptoms often worsen, with patients experiencing redness, swelling, eye irritation, and changes in eye position. This is the most crucial time for treatment, as interventions are most effective at preventing permanent damage. The disease then enters a plateau or stabilization phase, where symptoms neither worsen nor improve significantly as inflammation begins to decrease. The duration of this phase varies by individual.
Finally, thyroid eye disease reaches the inactive phase, where active inflammation subsides but any structural changes, such as eye protrusion, become permanent. While scarring of tissues may continue during this phase, this is typically when surgical corrections, if needed, are performed. It’s important to note that this progression can vary by individual, and does not always follow a straightforward path. Some patients experience periods of “flare-ups” of symptoms or reactivation of the active, inflammatory phase of the disease.
Smoking can worsen progression and extend the active phase, which is why early treatment during the active phase tends to give better outcomes. Frequent follow-up appointments with our physician for monitoring is essential throughout all phases to track changes so that treatment can be modified accordingly.
The risk factors for thyroid eye disease include genetic, lifestyle, and medical conditions. Women are more likely than men to develop the disease. Presentation of the disease has bimodal distribution, meaning it affects younger women and also middle-aged women. While uncommon for people over 80, there are patients who have had this in their 80s and even 90s. Some patients as young as 5 have been treated for the disease.
The Rundle’s Curve is a graphical representation of TED’s typical progression. It illustrates the phases of thyroid eye disease – initial trigger through active inflammation to eventual fibrosis. It highlights the importance of early intervention in the prevention of irreversible damage.
The risk factors for thyroid eye disease include genetic, lifestyle, and medical conditions. Women are more likely than men to develop the disease.
Presentation of the disease has bimodal distribution, meaning it affects younger women and also middle-aged women. While uncommon for people over 80, there are patients who have had this in their 80s and even 90s. Some patients as young as 5 have been treated for the disease. Those with a family history of thyroid or autoimmune disorders face increased risk, and Hispanic and Asian ethnicities may experience more severe disease presentation.
Smoking is the most significant modifiable risk factor, with both direct smoking and secondhand smoke exposure increasing likelihood and severity. High stress levels and poor sleep patterns can also contribute to disease development.
Having Graves’ disease is the most common precondition, while other autoimmune conditions, radioactive iodine treatment (for thyroid disorders), and abnormal thyroid levels can also increase risk. Environmental factors which are known to trigger autoimmune responses are often a precursor to development of the disease. Additionally, pregnancy and major hormonal changes can trigger or worsen thyroid eye disease, as can the use of certain hormone medications. Smokers not only have a higher risk of developing thyroid eye disease, most likely will experience more severe symptoms, longer active disease phases, and respond less favorably to treatment.
The diagnosis of thyroid eye disease begins with a detailed clinical examination. Your doctor(s) evaluate common signs like eye bulging (proptosis), eyelid retraction, and eye movement restrictions.
During this examination, they conduct vision tests to assess any impact on eyesight, measure eye pressure, and determine how far the eyes protrude. They also evaluate color vision and visual fields to check for any optic nerve compression.
Blood tests are necessary, including thyroid function tests (TSH, T3, T4) to check thyroid hormone levels and thyroid antibody tests, particularly TSI and TRAb. These tests help confirm the underlying autoimmune nature of the condition and influence treatment decisions. Imaging studies are often required, with CT scans of the orbits examining eye muscle enlargement and orbital tissue changes, while MRI scans can show soft tissue inflammation more clearly. These detailed images help determine disease severity and influence treatment strategies.
The diagnostic process also includes disease activity assessments. These assessments are particularly important for determining whether the disease is in an active inflammatory phase or has stabilized. Through this diagnostic approach, your doctor(s) can develop an individual treatment plan and effectively monitor your disease progression over time. The combination of clinical examination, laboratory testing, advanced imagery, and standardized assessments provides a complete picture of the condition’s severity and activity.

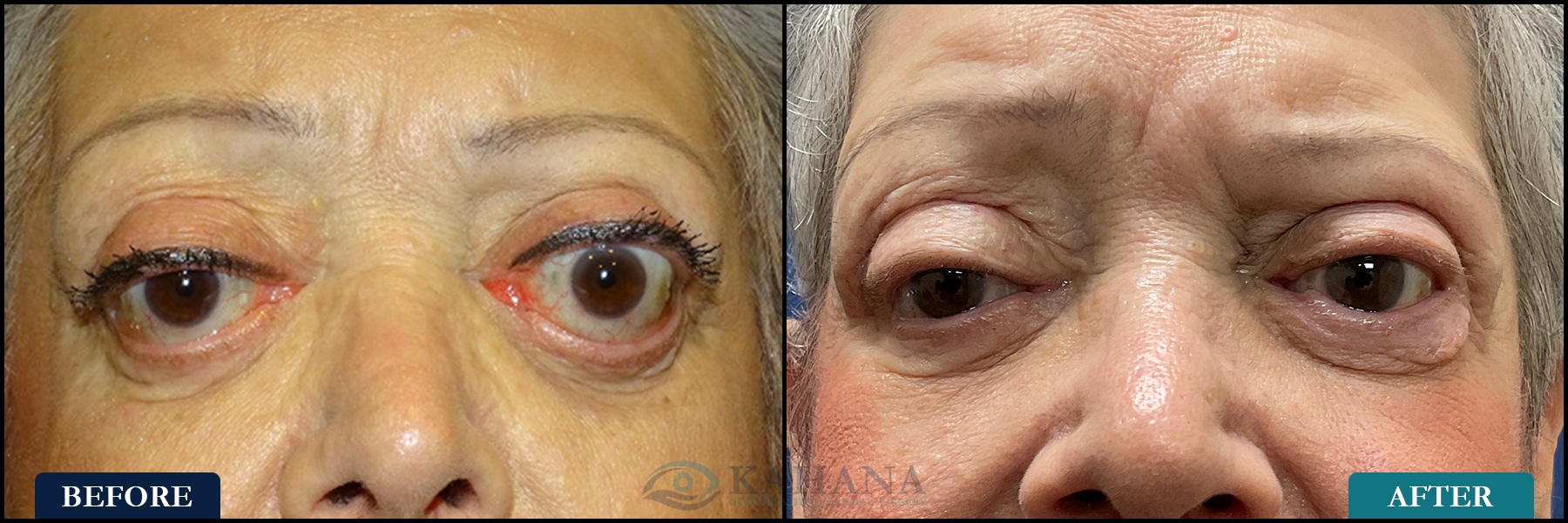
Treatment must be carefully timed and coordinated to maximize effectiveness and minimize complications. The approach differs depending on whether the disease is in its active phase or remission.
Treatment during the active phase of the disease focuses on preserving sight and the integrity of the cornea as well as providing treatment for double vision when it interferes with daily functioning and becomes bothersome.
Most patients experience relief from dry eyes by using artificial tears throughout the day and gels or ointments at night. Some patients also use eye covers at night or tape their eyes shut to keep them from becoming dry if the eyelids do not close properly. Dryness occurs because the lids are retracted and cannot blink properly, because the tear-producing glands have been affected by the autoimmune process and aren’t functioning well, and/or because the forward bulging of the eyes prevents them from being completely covered by the lids.
In some cases, acute swelling causing double vision or loss of vision may be treated for a limited time with oral prednisone. However, prednisone given for more than a few weeks at the dosages required to suppress the autoimmune inflammation always causes bothersome and dangerous side-effects that may become severe. In patients who respond to prednisone, a short course of intravenous (IV) steroids (methylprednisolone) may provide symptomatic improvement with fewer side effects than oral prednisone; this is referred to as an IV steroid pulse. Surgical decompression can also be used during the active phase, most often to relieve progressive damage to the optic nerve (optic neuropathy), but sometimes it can also be helpful in reducing orbital congestion, redness, pain, and eye exposure.
A newly FDA-approved drug, teprotumumab (Tepezza®, Horizon Therapeutics), has been shown to be effective in the majority of patients with active thyroid eye disease, i.e. patients who experience eye redness, pain with eye movement, worsening proptosis, and/or worsening diplopia. Teprotumumab is given by eight IV infusions over 24 weeks. It is very expensive, and requires insurance pre-authorization, but can be a very good option for some patients.
Learn More About Non-surgical Treatment Options
The remission phase offers opportunities to correct remaining problems through targeted interventions. Proper sequencing of treatments during this phase is crucial for optimal results.
Once the disease achieves remission and the thyroid hormone levels are stabilized, treatment can focus on restoring function and correcting unacceptable changes that persist after the ocular conditions of the active phase have stabilized, such as bulging eyes (proptosis), double vision (diplopia), and eyelid malposition. Treatment at this point is typically surgical, and needs to proceed in a predetermined order: orbital surgery first to correct the proptosis (orbital decompression), followed by eye muscle surgery to correct the diplopia, followed by eyelid surgery to improve eyelid closure and corneal protection.
It is critically important to stop smoking in order to reduce the severity and duration of thyroid eye disease.
The content above was originally published by: Kahana, Alon. “What Is Thyroid (Graves) Eye Disease???” North American Society of Academic Orbital Surgeons, 26 Sept. 2016, https://nasaos.org/what-is-thyroid-eye-disease/
We are a destination clinic for patients from throughout the Midwest and beyond, offering the latest surgical and non-surgical technologies and a deep understanding of this particularly dreadful disease process.
Dr. Kahana is an internationally renowned expert in thyroid eye disease – performing more than 250 orbital surgeries annually.
Patients travel from all over the United States and the world seeking his expertise and the care of his accomplished practitioners and staff. Dr. Kahana’s practice combines academic-level surgical innovation and customized treatment approaches with personalized patient care, while also offering access to clinical trials for thyroid eye disease management.
Dietary choices can significantly impact autoimmune disease activity. Understanding the relationship between diet and inflammation helps patients make informed food choices.
Patients who suffer from auto-immune inflammatory conditions, such as Graves disease, lupus, sarcoidosis, etc., need to be very cognizant about what they put into their bodies.
What we eat has a huge impact on our immune system. Many processed foods contain chemicals that can stimulate or suppress an immune response, and meats made from mammals (e.g. cows) contain proteins that mimic our own can exacerbate an auto-immune response.
For patients with auto-immune inflammatory conditions, I typically recommend a diet that is a variation of what’s been called the “caveman diet.” You should eat naturally occurring foods with minimal preservatives. And you should reduce beef and cow milk consumption to no more than once a week. After doing this for 3 months, you should expect to feel better and with fewer effects of your autoimmune condition. Maintaining this diet is not easy, but it’s worth it for your health.
Fluctuations in thyroid hormones can activate dormant embryological pathways, contributing to disease progression and emphasizes the importance of stabilizing thyroid function – prolonged hypothyroidism can be more detrimental to eye health than hyperthyroidism in this context.
Environmental factors can significantly impact disease progression and treatment outcomes. Understanding and modifying these factors can help improve treatment success.
Smoking contributes to TED progression through hypoxia-induced fibrosis. Additionally, the importance of vitamin D in immune regulation is discussed, with practical advice on supplementation, especially for those living in northern latitudes.
Dealing with thyroid eye disease is more than just a physical impairment – it’s an emotional obstical that can impacts your daily life. Many patients experience a very meaningful shift in life experience under treatment of a qualified physician.
Dr. Spadaro explains the timeline of clinical research, Teprotumumab (Tepezza®) development, and current clinical trials for thyroid eye disease.
Dr. Underwood discusses the benefits of an early thyroidectomy for preventing thyroid eye disease from worsening and to stabilize thyroid function more rapidly.
Dr. Kahana has taken special interest in thyroid eye disease throughout his career, having performed research on the molecular underpinnings of this complex disease.
Dr. Kahana is an internationally renowned expert in orbital and ophthalmic plastic surgery.
The providers and staff at Kahana Oculoplastic and Orbital Surgery are known for the care and concern they show toward their patients before, during, and after each procedure. Part of our commitment to innovation includes the opportunity for our patients to participate in clinical trials of novel medical therapies for thyroid eye disease. We also host regular patient-centered forums that help educate, engage and support patients and their families.
The team at Kahana Oculoplastic Surgery specializes in the treatment and management of thyroid eye disease.







