Scarring Disorders of the Conjunctiva

Join Us for the 2026 TED Patient Forum >> Register


The conjunctiva is the clear “skin” of the eyeball. It is crisscrossed by blood vessels and nerves, and covers the sclera (white of the eye) and insertions of the muscles that move the eye.
Inflammation or infection of the conjunctiva is referred to as “conjunctivitis,” which is commonly called “pink eye.” While conjunctivitis is usually a relatively mild and self-limiting condition, there are variations of inflammatory conjunctivitis that can cause permanent damage to the conjunctiva.
These include ocular cicatricial pemphigoid (OCP), Stevens Johnson Syndrome (SJS), Lichen Planus and other lichenoid conditions, pterygium, and amyloidosis. Lesions of the conjunctiva can also represent conjunctival cancer (neoplasm), so a thorough evaluation is always required.
At Kahana Oculoplastic and Orbital Surgery, we treat both inflammatory and neoplastic conditions of the conjunctiva.
Ocular cicatricial pemphigoid, or OCP, is a cicatrizing (scarring) condition affecting the conjunctival of the eyes. It is a type of autoimmune mucous membrane pemphigoid that leads to chronic inflammation of the ocular surface.
This chronic inflammation causes scarring of the conjunctiva and damage to all components of the tear film, leading to severe dry eye and corneal keratinization. Ultimately, if left untreated, OCP can lead to blindness.
Early disease presents as chronic conjunctivitis and dry eyes.
As the inflammation and fibrosis, or scarring, progresses, patients will exhibit symblephara (scar bands of the conjunctiva) and worsening keratinization of the ocular surface. Vision will decrease, and eye motility will decrease due to tethering of the eyelid to the ocular surface.
Clinical suspicion of the disease warrants a biopsy of the conjunctiva for diagnosis.
As this is a chronic, progressive disorder, treatment is strongly recommended. Co-management with a dermatologist who has experience in managing oral medication for OCP is recommended, along with management of the ocular complications. We will recommend initiation of ocular lubrication, along with additional therapy based on your clinical presentation and symptoms.
Ocular cicatricial pemphigoid often requires a multi-faceted approach to treatment. Long-term use of ocular lubrication is necessary, though often not adequate to maintain a healthy ocular surface and decrease the risk of pain and vision impairment.
At Kahana Oculoplastic Surgery, we offer many options for in-clinic and surgical intervention. Symblephara respond well to injected 5-Fluorouracil, however, may require surgical excision and reconstruction with amniotic membrane. In cases where the disease is more advanced, patients may also suffer from cicatricial entropion with eyelashes rubbing against their already fragile corneas.
Surgical repair of cicatricial entropion, sometimes warranting excision of the lash line, may be recommended. Additionally, placement of amniotic membrane to the fornices and ocular surface can help with corneal epithelial regeneration and decrease the inflammatory burden that is worsening fibrosis.
Ultimately, OCP is a chronic condition that impairs vision and causes discomfort. Not all patients experience the same rate of progression or severity, and a tailored approach by your providers is necessary. Long-term medical and surgical management is often required to maintain the ocular surface.
Stevens Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) are rare but very serious types of immune-mediated desquamating skin and mucous membrane disorders.
The difference between SJS and TEN depends on the percentage of body surface area involved. Both are caused by a reaction to medication, most often antiobiotics, anti-convulsants, or anti-inflammatories, however, they can be in response to any drug or even by your own body’s response to an infectious organism.
In most cases, there is ocular involvement and can present an ophthalmic emergency, with some cases leading to corneal ulceration, perforation, and blindness. These disorders require prompt and often ongoing treatment.
In cases of SJS and TEN, it is imperative to undergo an ophthalmic examination on presentation and throughout the course of hospitalization to determine the ocular involvement and risk. In the acute setting, placement of amniotic membrane is the best option for ocular involvement of SJS and TEN.
At Kahana Oculoplastic Surgery, we treat many patients who suffer from chronic complications of Sevens Johnson Syndrome and Toxic Epidermal Necrolysis, and offer a variety of options based on the patient’s individual presentation.
The common ocular manifestations of SJS and TEN include chronic conjunctivitis, limbal stem cell deficiency leading to worsening corneal involvement, severe keratoconjunctivitis sicca, symblephara formation, corneal scarring, shortened fornices, cicatricial entropion or destruction of lid margins, severe blepharitis, and more. Many patients have ongoing discomfort, light sensitivity, and decreased visual acuity.
Treatment includes a multi-faceted approach, including long-term use of lubricating or medicated eye drops, serum tears, recurrent placement of amniotic membrane, reconstruction of the ocular surface and/or fornices, excision and reconstruction of the lid margin, and more.
Some patients will ultimately require corneal transplant, and unfortunately, some patients will require removal of a blind eye with the placement of an implant and ocular prosthesis.
Stevens Johnson Syndrome and Toxic Epidermal Necrolysis are devastating skin and mucous membrane eruptions that occur in response to medications. Most cases include ocular involvement that can be severe and vision-threatening. It is our goal at Kahana Oculoplastic Surgery to treat each patient as an individual and assess their needs through a detailed exam and discussion of options. The priority in patients who suffer from Stevens Johnson Syndrome or Toxic Epidermal Necrolysis is to improve comfort and vision.
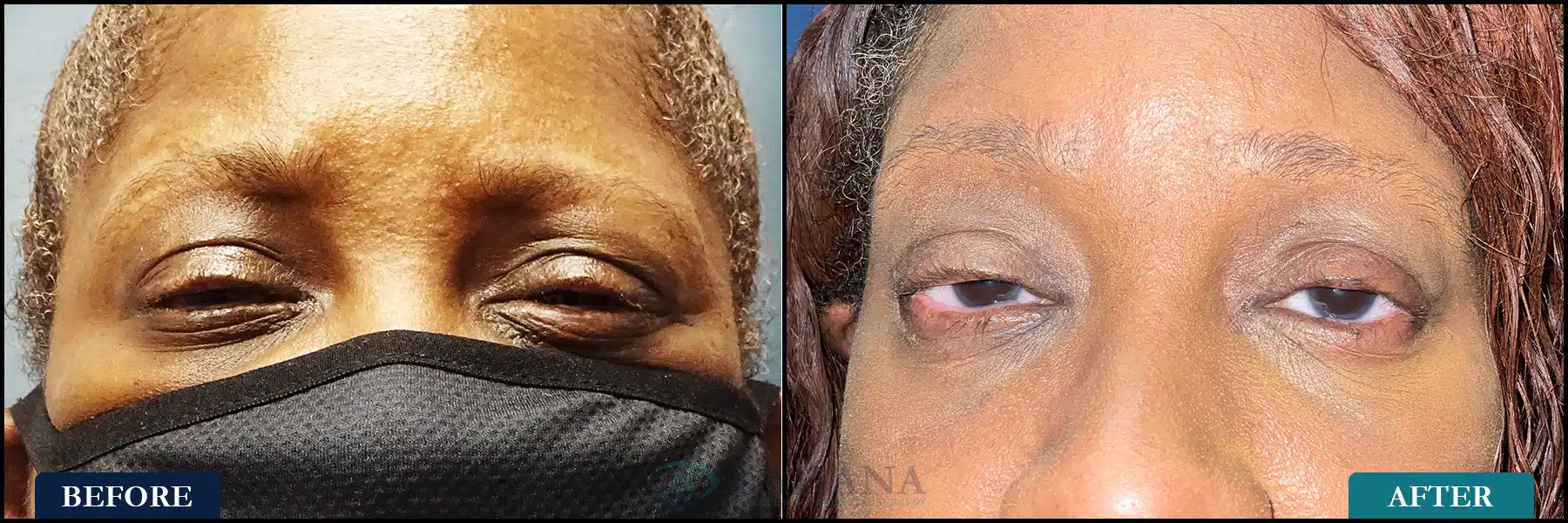
This is a patient with Stevens Johnson Syndrome who could hardly open her eyes when she first came to KOS due to eye pain and light sensitivity. She had a series of injections with 5FU, Acthar injections, and bilateral upper and lower eyelid fornix and lid margin reconstruction with buccal and amniotic membrane grafting. She now is comfortable, can open her eyes, and has significant improvement in vision. Post op over 1 year.


Options for treating scarring disorders of the conjunctiva are customized to the needs of the patient. It is not a “one size fits all” approach.
In order to best help each of our patients, a thorough exam and discussion of options are required. Oftentimes, this will include a step-wise approach, beginning with the initiation of non-surgical therapy and building upon these interventions as the patient’s symptoms and disease require.







